
The first phase might be due to the introduction of a potent vasoconstrictor arising from the amniotic fluid, and the second phase is thought to be due to a direct myocardial depressant also from the amniotic fluid. If even a small volume of amniotic fluid enters the maternal circulation, the initial haemodynamic response consists of acute pulmonary hypertension and vasospasm complicated by severe hypoxaemia and right-sided heart failure, followed by a second phase of more sustained left ventricular failure. Other cases have been associated with abdominal trauma, ruptured uterus or intrapartum amnioinfusion 7.Īmniotic fluid embolism (AFE) can occur only when there is a breech in the barrier between the amniotic fluid and maternal circulation. Our case was also one of these exceptions.Īlthough authors noted that patients were most likely to present during labour or shortly thereafter, there are several case reports of AFE occurring during Caesarean sections and therapeutic abortions as well as occasional cases in the late postpartum period, or very rarely in a non-labouring patient. Subsequent experiences have shown that there are a number of exceptions to this classical description. The use of uterine stimulants, meconium staining of the amniotic fluid or the presence of a large or dead fetus were also felt to increased the risk 6. The patient described in this case report had all of these factors.Īmniotic fluid embolism (AFE) was thought to more likely occur in the elderly multiparous patient who had an unusually strong or rapid labour or who had just delivered following such a labour. Both the United States and the United Kingdom have a national registry for suspected AFE, and entry criteria consist of the presence of the four following factors: 1) acute hypotension or cardiac arrest 2) acute hypoxia 3) coagulopathy or severe clinical hemorrhage in the absence of other explanations 4) all of these occurring during labour, Cesarean delivery, or dilatation and evacuation (D & E) or within 30 min postpartum with no other explanation for the findings 5. 
AFE should be suspected in any pregnant patient, specifically those with ruptured membranes, who develop sudden onset dyspnea with hypoxia, acute hypotension and/or cardiac arrest followed by a profound coagulopathy. 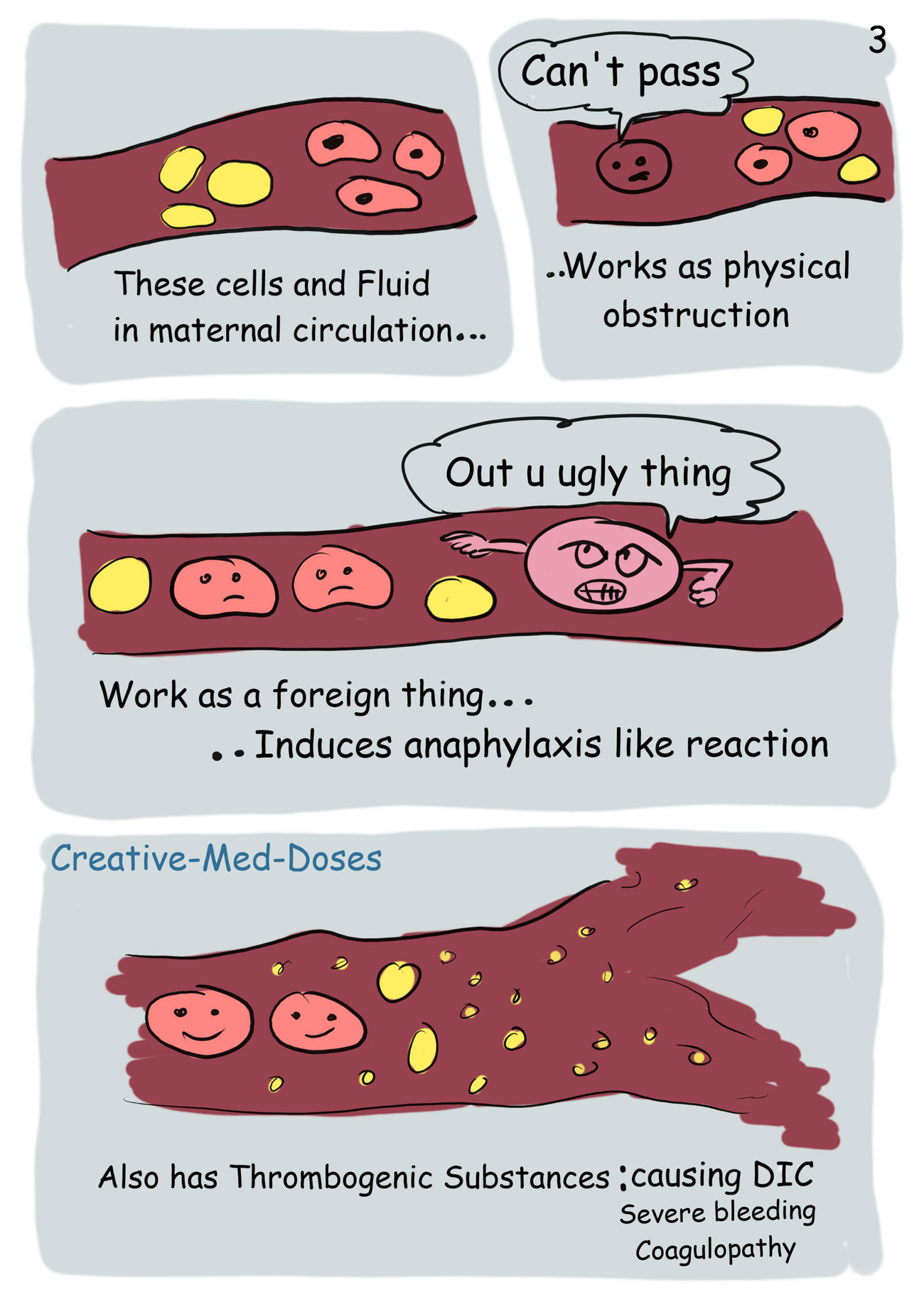 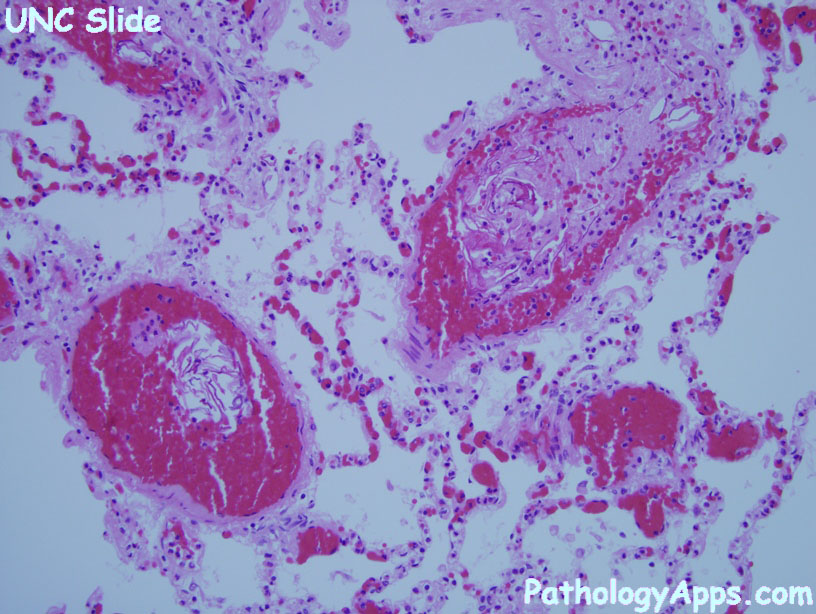
The differential diagnosis includes air or thrombotic pulmonary emboli, septic shock, aspiration pneumonia, acute myocardial infarction, placental abruption, eclampsia, complication of tocolytic therapy with β-sympathomimetics, transfusion reaction and local anaesthetic toxicity 4. Any condition that presents as acute cardiorespiratory collapse or massive hemorrhage in the peripartum period must be systematically evaluated. The diagnosis is therefore made by exclusion of other causes. The diagnosis of AFE is based on its clinical presentation and supportive laboratory studies. There is no one specific test that can confirm this syndrome. Autopsy was not performed.Īmniotic fluid embolism (AFE), first described by Meyer in 1926, is a topic of great concern in obstetrics today because of its dramatic presentation and high rate of mortality 3. The patient was declared dead 40 minutes after the onset of resuscitative efforts. Then, maternal bradycardia and asistoli was developed and cardiopulmonary resuscitation (CPR) was performed. During operation, the patient developed severe haemorrhage and shock necessitating massive blood transfusion. Caesarean section was performed immediately, but the male baby died. Supportive measures, including fluid resuscitation, inotropic support and plasma, were administered. Cardiotocography revealed signs of foetal distress and ultrasound showed oligohydramnios of the foetus. Laboratory values revealed mild coagulopathy. A central venous catheter was inserted in the right internal jugular vein and central venous pressure was 8 mmHg. She was transferred to intensive care unit. Endotracheal intubation was immediately performed, and the patient was mechanically ventilated. The electrocardiogram showed only a sinus tachycardia. The chest x-ray revealed central bilateral pulmonary oedema. Arterial blood gas analysis showed a severe hypoxaemia. She was semi-orientated, tachycardic, tachypnoeic, dyspnoeic, hypotensive and cyanotic. Vaginal examination revealed a cervix dilated 3-4 cm, effaciated 60%, and the fetal head stated at minus 2. Her antepartum obstetric history was unremarkable, but her past medical history was significant for a diagnosis of asthma and some drug allergies. A 32-year-old nulliparous woman at 40 weeks' of gestation, was admitted to the our emergency service with complaints of vaginal bleeding and pain.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
